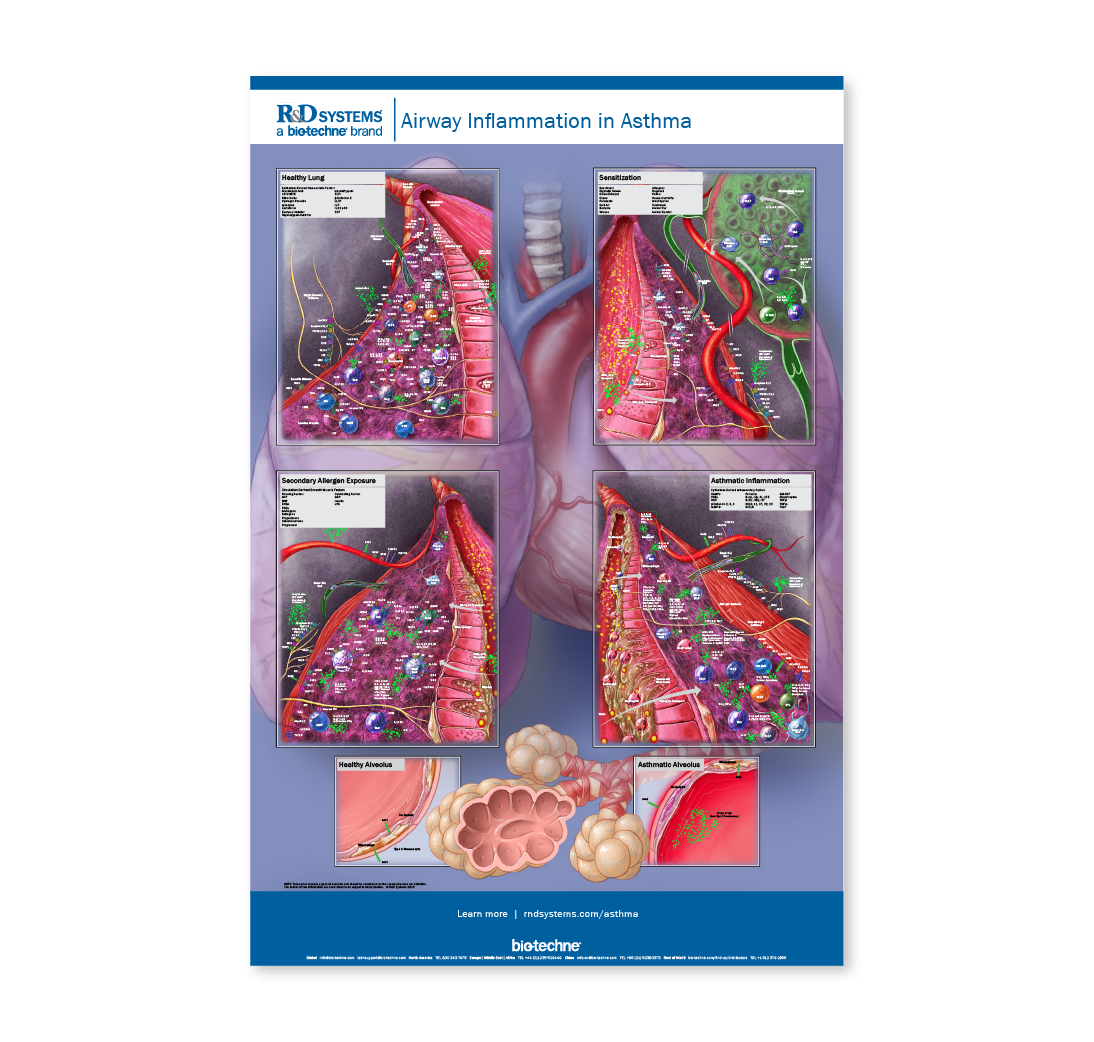
Airway Inflammation In Asthma
Life Science PostersAsthma is a complex disease with serious complications of inflammation and airway constriction. Many allergens are proteolytically active and can degrade adhesion molecules in epithelial cell tight junctions. Protease activated receptors (PARs) and microbial antigen activated TLRs trigger inflammatory cytokine release. Particulate or gaseous pollutants such as cigarette smoke, diesel exhaust, and ozone bind to airborne allergens, enhance their uptake into the airway epithelium, and promote the development of allergic immune responses. For an interactive phenotyping and marker guide to these cells, please see our Airway Inflammation of Asthma Cells resource.
Allergens are trapped and presented by dendritic cells which traffic to draining lymph nodes for interaction with naïve T cells. Allergic immune responses are Th2 biased and are dominated by the cytokines IL-4, -5, -9, and -13. Th2 cells and IgE-producing plasma cells home to the airway lamina propria where a secondary exposure to the same allergen triggers a massive expansion of the immune response. Additional immune cells are recruited, notably basophils, eosinophils, mast cells, and ILC2. Non-allergic immune responses in asthma are characterized by the infiltration of Th1 and Th17 cells and the production of IFN-gamma, IL-1, -6, -12, -17, and TNF-alpha.
In both allergic and non-allergic asthma, airway hyperresponsiveness is triggered by prostaglandins, leukotrienes, adenosine nucleotides, histamine, and neurokinins. These mediators are released by leukocytes and sensory C-fibers that innervate the airway. They trigger smooth muscle contraction, enhanced activity in the C-fiber, and continued support of the immune response. Remodeling of the airway is defined by increased smooth muscle proliferation and fibrosis of the basement membrane. Epithelial goblet cells also hyperproliferate and upregulate mucin release into the airway lumen. Inflammation, smooth muscle contraction, and mucus hyperproduction all contribute to airway narrowing and shortness of breath.
Related Information
| Allergy, Asthma and Inflammation | Basophils | Chemokines and Receptors |
| Cytokines and Receptors in Allergy and Asthma | Eicosanoids and Regulators | Eosinophils |
| Group 2 ILCs | Mast Cells | Th2 Cells |