Hemopexin (HPX) is a 60 kDa plasma glycoprotein with two four-bladed beta -propeller folds. This structural motif has been found in other proteins including collagenases and provides sites for protein-protein interactions (1‑3). The liver is the major synthesizing organ. Expression in the central nervous system, in the retina, and in peripheral nerves has also been observed. Hemopexin belongs to the family of the acute-phase proteins whose synthesis is induced after an inflammatory event. Hemopexin participates in maintaining and recycling the iron pool by utilizing its high binding affinity toward heme composed of protoporphyrin IX and iron. It also functions in preventing oxidation caused by heme after hemolysis. Hydrophobic heme molecules can intercalate into lipid membranes and participate in the oxidation of lipid membrane components through the Fenton reaction resulting in lipid peroxidation. Hemopexin undergoes a conformational change upon the binding of heme. The conformational change allows hemopexin to interact with a specific receptor, forming a complex which is then internalized. In the plasma, it is likely that heme binds albumin (35‑55 g/L) first because of the higher concentration of albumin in plasma than hemopexin (0.5‑1.2 g/L), and is then transferred to hemopexin, which has a much higher affinity (Kd ~ 1 pM) toward heme. Heme concentrations in plasma increase after hemolysis, which is associated with several pathological conditions such as reperfusion injury and ischemia.

Key Product Details
Species Reactivity
Human
Applications
Immunohistochemistry
Label
Unconjugated
Antibody Source
Polyclonal Sheep IgG
Loading...
Product Specifications
Immunogen
Mouse myeloma cell line NS0-derived recombinant human Hemopexin
Thr24-His462
Accession # P02790
Thr24-His462
Accession # P02790
Specificity
Detects human Hemopexin in direct ELISAs.
Clonality
Polyclonal
Host
Sheep
Isotype
IgG
Scientific Data Images for Human Hemopexin Antibody
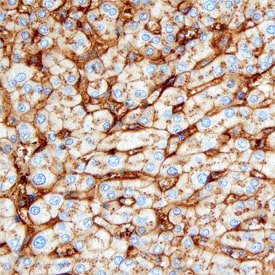
Hemopexin in Human Liver.
Hemopexin was detected in immersion fixed paraffin-embedded sections of human liver using Sheep Anti-Human Hemopexin Antigen Affinity-purified Polyclonal Antibody (Catalog # AF4490) at 3 µg/mL overnight at 4 °C. Before incubation with the primary antibody, tissue was subjected to heat-induced epitope retrieval using Antigen Retrieval Reagent-Basic (Catalog # CTS013). Tissue was stained using the Anti-Sheep HRP-DAB Cell & Tissue Staining Kit (brown; Catalog # CTS019) and counter-stained with hematoxylin (blue). Specific staining was localized to bile canaliculi. View our protocol for Chromogenic IHC Staining of Paraffin-embedded Tissue Sections.Applications for Human Hemopexin Antibody
Application
Recommended Usage
Immunohistochemistry
5-15 µg/mL
Sample: Immersion fixed paraffin-embedded sections of human liver
Sample: Immersion fixed paraffin-embedded sections of human liver
Formulation, Preparation, and Storage
Purification
Antigen Affinity-purified
Reconstitution
Sterile PBS to a final concentration of 0.2 mg/mL. For liquid material, refer to CoA for concentration.
Loading...
Formulation
Lyophilized from a 0.2 μm filtered solution in PBS with Trehalose. *Small pack size (SP) is supplied either lyophilized or as a 0.2 µm filtered solution in PBS.
Shipping
Lyophilized product is shipped at ambient temperature. Liquid small pack size (-SP) is shipped with polar packs. Upon receipt, store immediately at the temperature recommended below.
Stability & Storage
Use a manual defrost freezer and avoid repeated freeze-thaw cycles.
- 12 months from date of receipt, -20 to -70 °C as supplied.
- 1 month, 2 to 8 °C under sterile conditions after reconstitution.
- 6 months, -20 to -70 °C under sterile conditions after reconstitution.
Calculators
Background: Hemopexin
References
- Tolosano, E. and Altruda, F. (2002) DNA and Cell Biol. 21:297.
- Mauk, M. R. et al. (2007) Nature Pro. Rep. 24:523.
- Ascenzi, P. et al. (2005) IUMB Life. 57:749.
Alternate Names
Beta-1B-glycoprotein, HPX
Gene Symbol
HPX
UniProt
Additional Hemopexin Products
Product Documents for Human Hemopexin Antibody
Certificate of Analysis
To download a Certificate of Analysis, please enter a lot or batch number in the search box below.
Note: Certificate of Analysis not available for kit components.
Product Specific Notices for Human Hemopexin Antibody
For research use only
Related Research Areas
Customer Reviews for Human Hemopexin Antibody
There are currently no reviews for this product. Be the first to review Human Hemopexin Antibody and earn rewards!
Have you used Human Hemopexin Antibody?
Submit a review and receive an Amazon gift card!
$25/€18/£15/$25CAN/¥2500 Yen for a review with an image
$10/€7/£6/$10CAN/¥1110 Yen for a review without an image
Submit a review
Protocols
Find general support by application which include: protocols, troubleshooting, illustrated assays, videos and webinars.
- Antigen Retrieval Protocol (PIER)
- Antigen Retrieval for Frozen Sections Protocol
- Appropriate Fixation of IHC/ICC Samples
- Cellular Response to Hypoxia Protocols
- Chromogenic IHC Staining of Formalin-Fixed Paraffin-Embedded (FFPE) Tissue Protocol
- Chromogenic Immunohistochemistry Staining of Frozen Tissue
- ClariTSA™ Fluorophore Kits
- Detection & Visualization of Antibody Binding
- Fluorescent IHC Staining of Frozen Tissue Protocol
- Graphic Protocol for Heat-induced Epitope Retrieval
- Graphic Protocol for the Preparation and Fluorescent IHC Staining of Frozen Tissue Sections
- Graphic Protocol for the Preparation and Fluorescent IHC Staining of Paraffin-embedded Tissue Sections
- Graphic Protocol for the Preparation of Gelatin-coated Slides for Histological Tissue Sections
- IHC Sample Preparation (Frozen sections vs Paraffin)
- Immunofluorescent IHC Staining of Formalin-Fixed Paraffin-Embedded (FFPE) Tissue Protocol
- Immunohistochemistry (IHC) and Immunocytochemistry (ICC) Protocols
- Immunohistochemistry Frozen Troubleshooting
- Immunohistochemistry Paraffin Troubleshooting
- Preparing Samples for IHC/ICC Experiments
- Preventing Non-Specific Staining (Non-Specific Binding)
- Primary Antibody Selection & Optimization
- Protocol for Heat-Induced Epitope Retrieval (HIER)
- Protocol for Making a 4% Formaldehyde Solution in PBS
- Protocol for VisUCyte™ HRP Polymer Detection Reagent
- Protocol for the Preparation & Fixation of Cells on Coverslips
- Protocol for the Preparation and Chromogenic IHC Staining of Frozen Tissue Sections
- Protocol for the Preparation and Chromogenic IHC Staining of Frozen Tissue Sections - Graphic
- Protocol for the Preparation and Chromogenic IHC Staining of Paraffin-embedded Tissue Sections
- Protocol for the Preparation and Chromogenic IHC Staining of Paraffin-embedded Tissue Sections - Graphic
- Protocol for the Preparation and Fluorescent IHC Staining of Frozen Tissue Sections
- Protocol for the Preparation and Fluorescent IHC Staining of Paraffin-embedded Tissue Sections
- Protocol for the Preparation of Gelatin-coated Slides for Histological Tissue Sections
- TUNEL and Active Caspase-3 Detection by IHC/ICC Protocol
- The Importance of IHC/ICC Controls
- Troubleshooting Guide: Immunohistochemistry
- View all Protocols, Troubleshooting, Illustrated assays and Webinars
Loading...
